A Step-by-Step Guide to Taking Vital Signs
Understanding the Importance and Techniques of Measuring Vital Signs

Vital signs are critical health indicators used extensively in healthcare for diagnosis and treatment guidance. These indicators, including pulse, respiration, temperature, and blood pressure, are measured in medical checkups and emergencies and can even be monitored at home. Acquiring proficiency in this skill is paramount for patient and medical professional safety.
Vital signs are indispensable in healthcare, providing essential insights into organ function and overall internal health. Adhering to proper techniques when measuring a patient’s vital signs is crucial.
This article delves into the technicalities and significance of measuring vital signs, a fundamental skill for medical personnel.
Related: Click here for our complete list of the most common Dental Assisting duties and responsibilities.
Related: Click here for our complete list of the most common Medical Assisting duties and responsibilities.
What Are Vital Signs?
Vital signs comprise four key health indicators: pulse, respiration, temperature, and blood pressure. These elements are more than just numbers; they are critical snapshots providing healthcare professionals with insights into a patient’s core bodily functions. Each sign serves as a piece of a puzzle that, when pieced together, presents a comprehensive picture of a patient’s current health status.
- Pulse: This measures the heart rate and rhythm, indicating the heart’s health and overall circulatory system efficiency. An irregular or abnormal pulse can indicate cardiac issues or other systemic health problems.
- Respiration: Observing the rate, depth, and pattern of breaths, respiration metrics can reveal issues related to lung function and oxygenation and can even signal distress or anxiety.
- Temperature: Body temperature is a crucial indicator of metabolic and thermoregulatory function. Abnormal temperatures can indicate infections, inflammations, hormonal imbalances, or reactions to medication.
- Blood Pressure: This measures the force of blood against artery walls and can indicate cardiovascular health, risk of stroke, and other conditions like hypertension or hypotension.
These vital signs are interconnected and can influence each other, highlighting the importance of viewing them collectively for a holistic understanding of a patient’s health.
What is the Purpose of Taking Vital Signs?
- Assessing General Physical Health:
- Vital signs are fundamental in routine health assessments. They provide a baseline that helps compare current measurements with past records to detect deviations from a patient’s normal range.
- Regular monitoring of vital signs can preemptively alert to health issues even before symptoms become apparent, allowing for early intervention.
- Identifying Signs of Potential Diseases:
- Vital signs are often the first indicators of underlying health issues. For example, a spike in temperature might indicate an infection, while a drop could suggest exposure or hypothermia.
- Changes in blood pressure or pulse rate can hint at cardiovascular issues, stress responses, or other systemic conditions.
- Monitoring respiration assists in detecting respiratory diseases, anxiety disorders, or even metabolic imbalances.
- Monitoring Recovery Progress:
- Post-surgery or during treatment for various conditions, vital signs are critical in tracking a patient’s recovery and response to treatment.
- Consistent or improving readings often indicate effective treatment and recovery, while fluctuations or deteriorations might necessitate a change in medical approach or further investigation.
In summary, vital signs are more than just measurements; they are invaluable tools in diagnosing, monitoring, and managing health and diseases. Their regular assessment is integral to patient care, ensuring timely and appropriate medical responses.
How Long Does it Take to Take Vital Signs?
The duration for measuring vital signs can vary from three to five minutes, depending on the specific sign and method used. This variation is due to the different techniques and tools required for each vital sign.
- Pulse Rate Measurement: A healthcare provider will typically measure the pulse by counting heartbeats for a full minute to ensure accuracy. However, a quicker method involves counting for 15 seconds and multiplying the number by four to estimate the beats per minute. This approach provides a snapshot of the heart’s rhythm and rate, which is crucial for assessing cardiovascular health.
- Temperature Assessment: Modern medical technology offers swift and efficient ways to measure body temperature. Certain digital thermometers can deliver accurate readings in as little as 30 seconds. This rapid measurement is essential in fast-paced medical settings or situations where a quick assessment is needed.
Overall, the process of taking vital signs is a balance between thoroughness and efficiency. Accurate measurement is critical to providing a reliable health status overview, but it is equally important to perform these checks promptly, especially in emergencies or during routine check-ups where time is a factor.
Who Can Take Vital Signs?
Measuring vital signs is a fundamental skill many healthcare professionals are equipped to perform. This group includes, but is not limited to, Emergency Medical Technicians (EMTs), paramedics, medical assistants, dental assistants, nurses, and physicians. Each role involves a keen understanding of what vital sign readings mean and how they can indicate a patient’s overall health status.
Expanding the Scope to Dental Practices
In the context of dental care, incorporating the measurement of vital signs is not a routine practice but offers significant advantages. Dentists and dental assistants can use these measurements to identify potential medical emergencies requiring prompt attention, ensuring patient safety and well-being during dental treatments.
- Pulse Rate Evaluation by Dental Assistants: Dental assistants must be vigilant when measuring a patient’s pulse rate. They should be aware of the normal pulse rate ranges – typically 70 to 120 beats per minute for children and 60 to 100 beats per minute for adults – and be able to recognize when a pulse is unusually weak or strong, which could indicate underlying health issues.
- Respiration Rate Monitoring: After recording the pulse rate, a dental assistant can measure the respiration rate by counting the number of breaths a patient takes in 15 seconds and multiplying this number by four to get the breaths per minute. The normal range for a healthy adult lies between 12 and 20 breaths per minute. This measurement is a vital indicator of respiratory health.
- Temperature Checks in the Dental Office: In the wake of the COVID-19 pandemic, it’s become increasingly common for dental assistants to take patients’ temperatures. An orally measured temperature of 98.6 degrees Fahrenheit is typically considered normal for a healthy adult.
- Blood Pressure Assessment: Monitoring a patient’s blood pressure involves paying close attention to systolic and diastolic pressures. Dental assistants should be familiar with the healthy blood pressure ranges for adults and children, as these readings can be crucial indicators of cardiovascular health.
Related: Go here to learn how to become a Dental Assistant.
Training Requirements for Taking Vital Signs
The pathway to becoming adept at measuring vital signs is diverse and can differ significantly based on geographical location and the specific healthcare field one is pursuing. The level and type of training required are tailored to ensure that professionals have the theoretical knowledge and practical skills necessary for accurately assessing these critical health indicators.
Specialized Training for Dental Assistants
- Formal Education and Certification: Dental Assistants, in particular, are generally expected to complete an accredited educational program and successfully pass a certification examination. This standardized approach ensures a comprehensive understanding and competency in dental-specific tasks and broader clinical skills like vital sign measurement.
- On-the-Job Training: Alternatively, some Dental Assistants may acquire these skills through hands-on training in a dental office setting. This method allows for practical learning and application of vital sign measurement in real-world scenarios, complementing their theoretical knowledge.
- Duration and Curriculum of Dental Assistant Programs: Typically, these programs span about a year or less, offering a blend of classroom instruction and clinical practice. This structure provides a well-rounded educational experience, covering all aspects of dental assistance, including the crucial component of vital sign measurement.
- Accreditation and Quality Assurance: Over 250 Dental Assisting programs across the United States are accredited by the Commission on Dental Accreditation (CODA). This accreditation is a hallmark of quality and ensures that the curriculum meets the high standards for producing competent and skilled dental assistants.
Vital Sign Procedures
Becoming proficient in taking vital signs is a process that requires dedication, practice, and an understanding of the correct techniques. This skill is essential in various healthcare settings, including occasionally in dental offices, and is critical for patient assessment and care.
Preparation for Vital Sign Measurement
- Training and Compliance: It’s essential to have proper training and be aware of your employer’s policies regarding vital sign measurement. Even in settings where this is rare, such as dental offices, being prepared is critical.
- Creating a Calm Environment: Ensure the patient is relaxed and comfortable before you start, as stress can affect vital sign readings.
Step-by-Step Guide to Measuring Vital Signs
Here are the general guidelines you should follow:
-
Pulse Measurement:
- Start by washing your hands thoroughly.
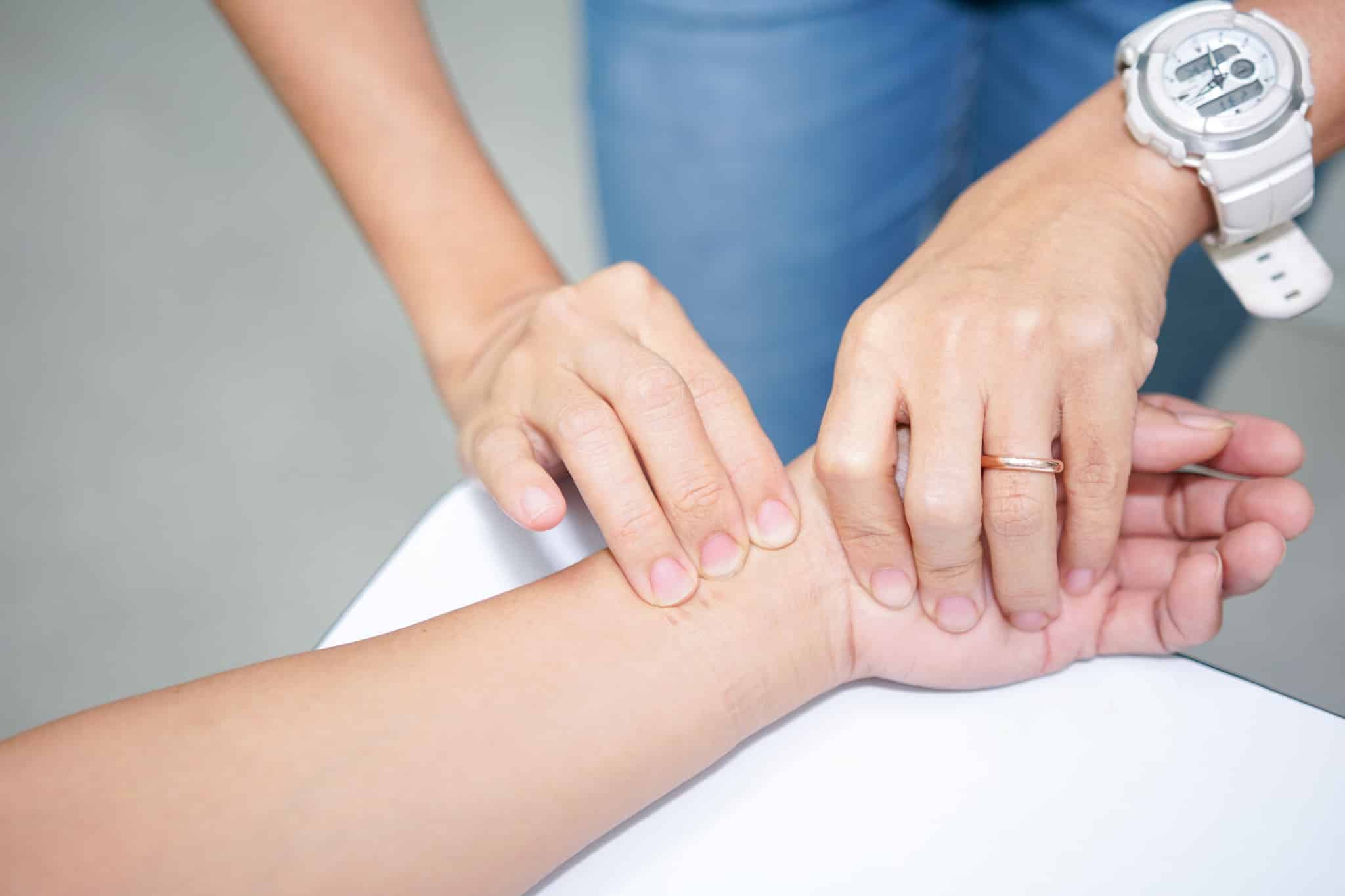
- Find the patient’s pulse using the radial artery located on the inside of the wrist near the thumb.
- Use your first two fingertips (not the thumb) to gently feel the pulse.
- Observe a clock or watch, timing your count with the seconds hand.
- Count the beats for a full minute for accuracy.
- Focus on the pulse beats rather than continuously watching the clock.
-
Respiration Rate:
- Again, ensure your hands are clean.
- Lightly place your fingers on the patient’s wrist.
- Count the number of breaths for one minute, remembering that a full breath includes both an inhale and an exhale.
- Note any additional observations, such as wheezing or signs of distress.
-
Temperature Measurement with a Digital Thermometer:
- Wash your hands and use a clean thermometer with a disposable cover.
- Activate the thermometer and place it under the patient’s tongue, asking them to close their mouth.
- After the beep, remove the thermometer and record the temperature.
- Clean and sterilize the thermometer after use.
-
Blood Pressure Measurement:
- Start with clean hands and a disinfected stethoscope.
- Confirm the blood pressure monitor is functioning properly.
- Locate the brachial pulse on the patient’s arm.
- Wrap the cuff around the arm, above the brachial pulse.
- Inflate the cuff to the specified level (usually until the dial reads 170).
- Slowly release the air, listening for the first and last thumps (systolic and diastolic pressure).
- Document the readings and any unusual findings.
Post-Measurement Recovery
While measuring vital signs typically doesn’t cause side effects, some patients may experience temporary discomfort, such as dizziness or minor bruising from blood pressure cuffs. This is often due to an improperly fitted cuff rather than the measurement process itself.

Essential Tools for Accurate Vital Sign Measurement
For healthcare professionals, having the right equipment is crucial for accurately measuring vital signs. These tools facilitate a comprehensive evaluation of a patient’s health status. Here’s a breakdown of the essential equipment:
- Thermometers: These are indispensable for measuring body temperature. Modern thermometers range from traditional mercury types to advanced digital models, providing quick and accurate readings.
- Stethoscopes: A fundamental tool in any medical kit, stethoscopes are used to listen to internal sounds of the body, particularly heartbeats and lung sounds, which are key indicators of cardiovascular and respiratory health.
- Blood Pressure Devices: Measuring blood pressure is vital, and devices like sphygmomanometers (manual blood pressure cuffs with a gauge) or digital blood pressure monitors are used. They help in detecting conditions like hypertension or hypotension.
- Combo Kits (Stethoscope + Blood Pressure): These kits, combining a stethoscope and a blood pressure cuff, are a convenient option. They are particularly useful for professionals who need to conduct comprehensive assessments frequently.
- Pulse Oximetry: This non-invasive tool measures the oxygen saturation level of the blood. It’s essential for monitoring patients’ oxygen levels, especially in critical care.
- Electrocardiogram (ECG) Machines: ECGs are crucial for assessing the heart’s electrical activity. They can identify various cardiac issues, from minor irregularities to severe conditions.
- Penlights: Used for examining areas like the eyes, mouth, and throat, penlights are a critical diagnostic tool. They assist in checking pupil response and oral health, which can indicate various health conditions.
Each of these tools play a specific role in the comprehensive assessment of vital signs, helping healthcare professionals diagnose and monitor their patients effectively.
What Are the Potential Risks or Complications of Taking Vital Signs
While seemingly straightforward, measuring vital signs carries significant responsibilities and potential risks if not done correctly. Accurate measurement of these signs is not just a routine task; it’s a critical component of patient care that can have far-reaching implications.
- The Gravity of Accurate Measurements: Healthcare professionals must measure vital signs with the utmost precision. Inaccurate readings can lead to misdiagnoses, resulting in inappropriate treatments or overlooking serious medical conditions. The consequences of such errors can range from minor health issues to life-threatening situations.
- Understanding the Impact: While taking vital signs may appear routine, its importance cannot be overstated. Each measurement provides crucial information about a patient’s health status. For instance, an undetected elevated blood pressure reading could overlook a risk of stroke or heart attack, while a missed low oxygen saturation might signal a respiratory or cardiac problem that requires immediate attention.
- Preventive Measures: To mitigate these risks, healthcare providers must be thoroughly trained in the correct techniques of measuring vital signs, stay updated with best practices, and use properly calibrated equipment. Additionally, it’s crucial to double-check readings that are out of the ordinary and consider the patient’s overall clinical picture.
- The Role of Vigilance: Healthcare professionals must remain vigilant and conscientious, understanding that each time they measure a patient’s vital signs, they play a crucial role in safeguarding their health and potentially saving lives.
In conclusion, the process of taking vital signs, while fundamental, demands accuracy and care. These measurements are indispensable tools in healthcare, serving as the first line of defense in identifying and responding to patient needs.
Advanced Techniques and Best Practices for Accurately Taking Vital Signs
Mastering the art of vital sign measurement is essential for healthcare professionals. Beyond basic practice and memorization, several advanced tips and best practices can enhance accuracy and ensure patient comfort during the process.
- Engaging Patient Cooperation:
- When measuring oral temperature, guide the patient to place the thermometer under their tongue. This ensures a proper placement for an accurate reading and minimizes discomfort.
- Knowledge of Temperature Variations:
- Understand the differences in temperature readings based on the method used. Oral temperatures may differ from rectal, tympanic (ear), or axillary (underarm) readings. Typically, rectal and tympanic temperatures are about 0.5 to 1.0 degrees Fahrenheit higher than oral readings, while axillary temperatures can be lower by the same range.
- Encouraging Patient Hydration:
- Advise patients to stay hydrated, especially before procedures like phlebotomy. Hydration can facilitate easier measurement of certain vital signs.
- Perfecting the Pulse Measurement Technique:
- Practice the right amount of pressure when taking a pulse. It’s crucial to balance firmness and gentleness to accurately feel the heartbeat without discomfort or slipping.
- Correct Positioning for Brachial Pulse:
- For an accurate brachial pulse, the patient’s arm should be straight. This position brings the artery closer to the surface, making it easier to locate and measure the pulse.
- Subtle Respiration Rate Counting:
- Discreetly count the patient’s respirations to prevent any conscious alterations in their breathing pattern. This can be done by pretending to continue measuring the pulse while actually observing their breaths.
- Ensuring Patient Relaxation:
- Accurate vital signs are best taken when the patient is calm and at rest. Ask patients to avoid eating, drinking, smoking, or exercising for at least 30 minutes before the measurement.
- Maintaining Hygiene and Equipment Care:
- Always wash hands before and after taking vital signs. Additionally, each piece of equipment should be cleaned and sanitized after use. Adhere to the manufacturer’s guidelines and your facility’s protocols for maintaining these tools.
By incorporating these advanced techniques into your practice, you can significantly improve the accuracy and reliability of vital sign measurements, contributing to better patient care and outcomes.

Why Should Dental Assistants Learn How to Take Vital Signs?
In the healthcare sector, the ability of Dental Assistants (DAs) to measure and understand vital signs is becoming increasingly valuable. While this skill might seem straightforward, its significance in ensuring patient health and safety is profound.
- Enhanced Patient Care: Dental Assistants who can accurately measure vital signs are better equipped to monitor a patient’s overall health. For instance, measuring blood pressure can be crucial, especially if a patient is nervous or has a history of hypertension.
- Proactive in Health Monitoring: In the era of COVID-19, temperature checks have become a standard procedure. Dental Assistants who can competently perform this task contribute to the safety of patients and staff by helping prevent the spread of illness.
- Preparedness for Emergencies: In a medical emergency in the dental office, a Dental Assistant with the ability to take and interpret vital signs becomes an invaluable asset. This skill allows for a quicker response and more informed decision-making during critical moments.
- Increased Team Efficiency: Dental Assistants skilled in vital sign measurement add significant value to the dental care team. Their ability to perform these assessments can streamline patient processing and enhance the overall efficiency of the practice.
- Career Advancement Opportunities: Acquiring and honing the skill of vital sign measurement can open up further professional opportunities for Dental Assistants. It demonstrates a commitment to comprehensive patient care and a readiness to take on additional responsibilities, which can be highly regarded in the healthcare field.
Learning and mastering vital sign measurement is beneficial and essential for Dental Assistants. It strengthens their role in patient care, prepares them for emergencies, enhances the functionality of the dental team, and can lead to greater career growth.
Start Your Career in Dental Assisting
Measuring vital signs is a critical skill aspiring Dental Assistants should consider learning for their careers. It’s also an essential practice for the diagnosis of various medical issues.
After all, vital signs measure your body’s essential functions and give medical professionals a window into the state of your health. Plus, they help physicians diagnose diseases, monitor the effects of treatments, determine medication dosages, and more.
If you’re inspired and want to pursue a medical career, Unitek College offers several healthcare programs, such as our Dental Assisting program.
Contact us today to learn more about our programs and tuition assistance options. Take the first step toward a rewarding future in healthcare!

